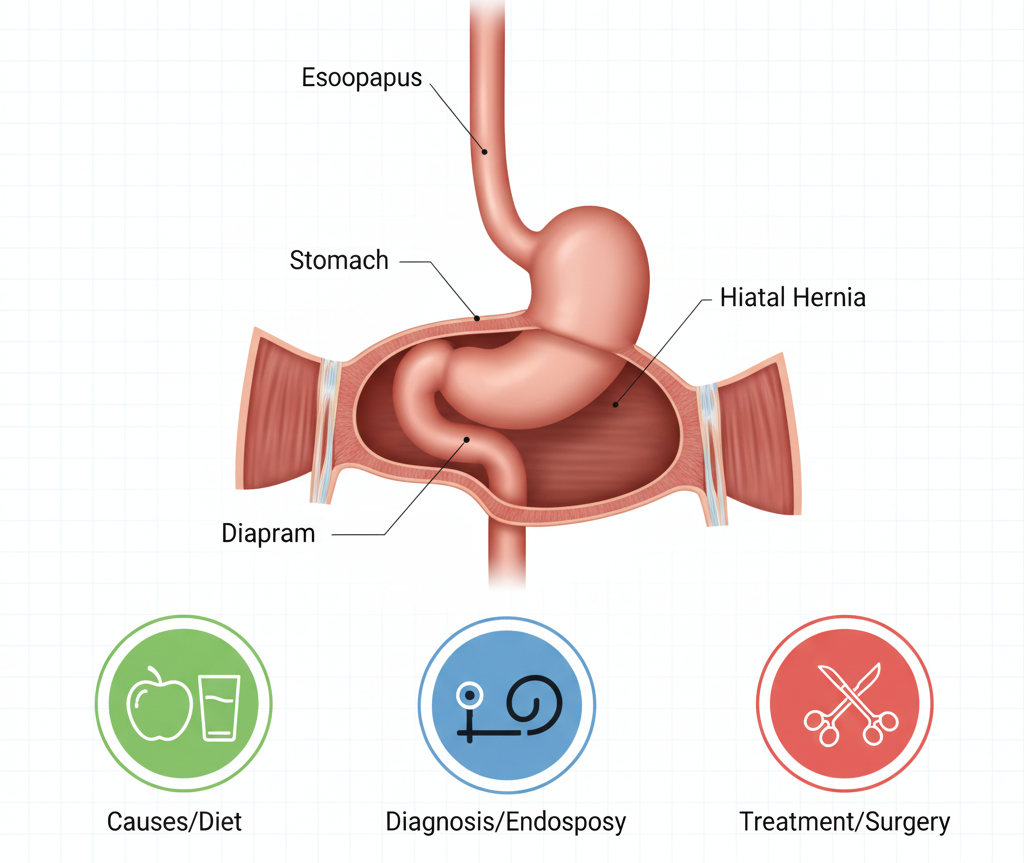
Hiatal Hernia for the Causes, Diagnosis, and Treatment Options
A hiatal hernia is a medical condition in which a portion of the stomach protrudes through the diaphragm into the chest cavity, often causing discomfort, acid reflux, or heartburn. Understanding its causes, including obesity, heavy lifting, or chronic coughing, is important for management, which may typically involve diagnosis with the use of imaging studies such as X-rays or endoscopy, followed by management, which could include lifestyle changes, medication, and surgical repair, depending on the severity.
Table of Contents
- Introduction to Hiatal Hernia
- Hiatal Hernia Develops for Understanding the Anatomy
- Types of Hiatal Hernia
- Common Causes of Hiatal Hernia
- Risk Factors and Most Affected Individuals
- Symptoms of a Hiatal Hernia
- How to Diagnose the Hiatal Hernia?
- Treatment Options for Hiatal Hernia
- Living With Hiatal Hernia: Long-Term Management Tips
- Conclusion
1. Introduction to Hiatal Hernia
It often comes with persistent heartburn, chest discomfort, or trouble swallowing, which many people mistake for a case of acid reflux. A hiatal hernia involves a part of your stomach bulging up through an opening in your diaphragm, where the esophagus goes through to connect to the stomach.
A hiatal hernia might sound minor, but it could bring about symptoms of acid reflux, regurgitation, and general pain. This article is going to take you through what goes on inside your body and how one can manage and treat this condition to find long-term relief for it.
2. Hiatal Hernia Develops for Understanding the Anatomy
A hiatal hernia may be easier to understand after learning a little about the diaphragm, which is the large dome-shaped muscle that separates your chest from your abdomen and helps you breathe.
The hiatus is a small opening in the diaphragm that the esophagus passes through on its way to joining your stomach. The stomach is normally inferior to the diaphragm and the esophagus is superior to the diaphragm.
A hiatal hernia can result from a weakening in the muscle tissue that allows the stomach to slide upward or be pushed upward into the chest cavity. This can disrupt the lower esophageal sphincter, the valve that prevents the regurgitation of stomach acid; thus, it causes acid reflux and other digestive symptoms.
3. Types of Hiatal Hernia
There are several variations of hiatal hernia, but two major types, explained below, determine the proper course of treatment.
3.1 Sliding Hiatal Hernia
This is the most common-one that happens in 95% of cases-in which the stomach and the lower esophagus slide up into the chest through the hiatus. It’s a temporary movement that can go back and forth, especially when lying down or after eating.
Common Symptoms:
- Heartburn
- Acid reflux
- Chest pain
- Regurgitation of food or liquids
Sliding hernias are often very responsive to lifestyle changes and medication.
3.2 Paraesophageal (Fixed) Hiatal Hernia
This is a more serious but less common type, comprising 5% of cases, in which a portion of the stomach pushes up alongside the esophagus and can become “stuck” in the chest. Since this may constrict blood flow to the stomach, it may need to be surgically corrected.
Common Symptoms:
- Chest pressure or pain
- Difficulty swallowing
- Feeling full sooner than usual after eating
- Shortness of breath
If a paraesophageal hernia is not treated, it can become
4. Common Causes of Hiatal Hernia
It is usually occur when there is increased pressure in the abdomen or weakness for diaphragm muscles, caused by one of the following:
- Age-related muscle weakness: With age, the diaphragm weakens and is more likely to herniate in older adults.
- Heavy lifting or straining: Activities that involve heavy lifting, bending, or straining increase the pressure in the abdomen.
- Prolonged coughing or vomiting: Long periods of coughing or vomiting can repeatedly strain the diaphragm.
- Obesity: It exerts pressure on the stomach and diaphragm.
Pregnancy may also displace the stomach upward with increasing abdominal pressure. Trauma of the chest or abdomen may lead to weakness of the diaphragm due to injury. Genetic predisposition: Some individuals are born with a larger hiatus that predisposes them to hernias. Though you cannot always prevent a hiatal hernia, keeping within a healthy weight and avoiding heavy strain can considerably reduce your risk.
5. Risk Factors and Most Affected Individuals
Hiatal hernias are found in everyone, though they are most commonly found in particular groups. This knowledge of who is most vulnerable aids in early detection and prevention.
- Age: Most cases occur in people over 50 because the muscles of the diaphragm weaken with age.
- Gender: Slightly more risk to women because of hormones and pregnancy.
The obesity problem usually involves increased intra-abdominal pressure, pushing the stomach upwards.
- Lifestyle Factors: These include smokers, individuals who have poor posture, and those who are sedentary.
- Genetic Factors: If hiatal hernias or related digestive disorders are in your family, you are at a greater risk.
By recognizing these risk factors early in their lives, people may have more avenues through which to monitor their digestive health, including healthy lifestyle habits.
6. Symptoms of Hiatal Hernia
The symptoms of a hiatal hernia depend on the type and the severity of the hernia. In some cases, there are no symptoms; in others, people experience symptoms related to acid reflux or GERD, which is Gastroesophageal Reflux Disease.
Common Symptoms:
- Heartburn (burning sensation in the chest)Regurgitation of food or acid into the mouth
- Chest pain often is mistakenly associated with heart disease.
- Difficulty swallowing or a feeling that food frequently becomes stuck in the throat
- Feeling full too quickly after eating Bloating and burping
- Shortness of breath, especially with large hernias
WHEN TO SEEK MEDICAL CARE
If you experience persistent heartburn, chest pain, or difficulty swallowing, seek medical attention. Severe pain that comes on suddenly, vomiting blood, or black stools indicate a serious complication and may require immediate medical intervention.
7. How to Diagnose the Hiatal Hernia?
It is based on a review of your medical history, physical exams, and imaging tests. Your doctor will most probably start by asking about your history and symptoms related to your digestion. It includes:
- Barium swallow (upper GI series): The patient drinks a chalky liquid called barium, which coats the inside of the esophagus and stomach. X-rays are then taken, which show the size and location of the hernia.
- Endoscopy: A small, flexible tube with a camera is passed down the throat for direct viewing of the esophagus and stomach to look for inflammation or ulcers.
- Esophageal manometry: This is a test that measures the strength and coordination of the esophageal muscles and lower esophageal sphincter.
- pH testing: A small probe measures the acidity of the esophagus to find out if acid reflux might be the cause of symptoms. Once accurately diagnosed, the right treatment can follow.
8. Treatment options for hiatal hernia
This Treatment will be based on the type and severity for hernia, with the milder forms treated with changes in the lifestyle and medications, while severe ones may require surgical intervention.
8.1 Lifestyle Modifications
For the Minor, consistent lifestyle changes can help alleviate symptoms:
- Eat smaller portions more often, rather than large meals.
- Avoid lie down immediately after eating; wait at least 2–3 hours.
- Elevate on the head of your bed to prevent nighttime reflux.
- Avoid trigger foods like spicy dishes, citrus, chocolate, and caffeine.
- Maintain the healthy weight to reduce the abdominal pressure.
- Stop smoking for the weakens the lower esophageal sphincter.
- Practice the light exercises and maintain good posture.
8.2 Medications
The following medications are often used to relieve discomfort and reduce acid production:
- Antacids for immediate relief.
- H2 receptor blockers, such as famotidine, which reduce acid production.
- PPIs, such as omeprazole, which can control acid for a longer period of time.
- These drugs do not fix the hernia.
- They only address the symptoms.
9. Living with Hiatal Hernia: Long-Term Management Tips
Living with a hiatal hernia does not need for life of the constant discomfort. Most individuals, with proper care, lead normal, healthy lives.
Here are some practical tips that could help in managing the condition for the long term:
9.1 Eat the Digestive-Friendly Diet
- Avoid food that trigger reflux such as onions, garlic, fried foods, alcohol.
- Eat slowly and chew thoroughly.
- Stay upright after meals.
- Include high-fiber foods that prevent constipation, which was a cause of increased abdominal pressure.
9.2 Maintain Body Weight
Extra weight put pressure on your stomach and diaphragm, so maintaining a healthy BMI can make a big difference.
9.3 Reduced Stress
Try relaxation techniques such as yoga, deep breathing, or meditation.
Stay Active
Gentle exercises, like walking, swimming, or stretching, improve digestion and strengthen the muscles of the diaphragm.
9.4 Sleep Smart
Use extra pillows or an adjustable bed to elevate the upper portion of your body during sleep, preventing upward flow of acid.
10. Conclusion
Although it may seem like such a serious condition, most people find that lifestyle changes, diet adjustments, and medication bring dramatic relief, while surgery to repair larger or more serious hernias often provides long-term relief.
By listening to your body, practicing healthier habits, and consulting with your doctor for persistent symptoms, you are on the pathway to living comfortably and preventing complications for years to come.



Post Comment